
Why Early Cancer Detection Matters More Than Ever in 2026: Health, Treatment, and Financial Considerations
13 Apr 2026
About this article:
- Understand why early cancer detection affects both treatment outcomes and total costs in Singapore.
- Learn how MediShield Life, Integrated Shield Plans, riders, and Critical Illness insurance support cancer care.
- Find out what cancer screening, diagnostics, and treatment are claimable under Singapore insurance frameworks.
- Get practical guidance on planning for cancer treatment expenses in the 2026 rider landscape.
Hearing the word “cancer” mentioned at any doctor’s appointment is never something anyone wants to hear. However, the rates of cancer have been rising globally. In 2022 alone, WHO reported 20 million new cancer cases. This number is expected to rise to 35 million by 2050. In Singapore, cancer is the leading cause of death, accounting for about 29% of all deaths. Approximately 1 in 4 to 5 Singapore residents will develop cancer in their lifetime.
Beyond its medical impact, cancer is also one of the most financially significant illnesses someone can face. From diagnostic scans and biopsies to surgery, chemotherapy, targeted therapy, and long-term follow-up, treatment costs can escalate quickly, particularly when cancer is detected at a later stage or requires ongoing therapy.
This means one thing is becoming clearer than ever:
Early detection does not just improve survival, it also reduces financial strain.
Cancer care in Singapore: Effective but not inexpensive
Singapore is well-known for having one of the best cancer outcomes in Asia. This is supported by our advanced diagnostics, specialist expertise, and access to modern therapies. Both Public and Private hospitals offer comprehensive cancer care, including precision diagnostics, multidisciplinary treatment planning, and access to targeted and immunotherapy drugs.
However, this level of care also reflects the true cost of modern oncology.
Cancer treatment costs vary widely depending on type and stage of the disease, but may include:
- Specialist consultations and investigations
- Imaging (CT, MRI, PET-CT)
- Surgery and hospitalisation
- Radiotherapy
- Chemotherapy cycles
- Targeted therapy or immunotherapy drugs
- Management of side effects and complications
- Long-term surveillance
Advanced systemic therapies alone can cost thousands per month. When treatment extends over months or years, the total cost can be substantial.
This is where your health insurance steps in. Insurance such as our Integrated Shield Plan, MediShield Life, Riders, Cancer Riders, and even your Corporate Insurance plays a critical role in making such care accessible.
Not sure if your plan covers what matters most?
Use the Hospital Bill Estimator to see what your expected
costs could be.
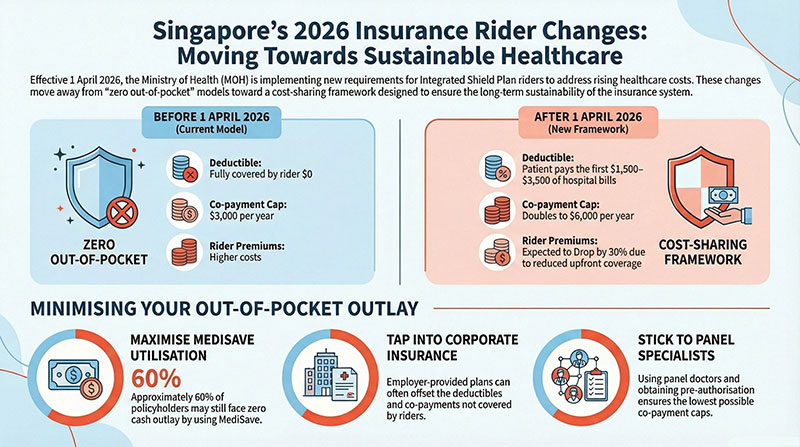
The 2026 Rider reset: Why patients will pay more upfront
If you have an Integrated Shield Plan and have utilised it, you will understand its importance and significance. Many policyholders also purchase riders to reduce or eliminate out-of-pocket costs such as deductibles and co-insurance.
However, from April 2026, Rider structures across insurers are changing.
Under the new framework:
- Deductibles (often $1,500–$3,500 for private hospital plans) can no longer be fully covered by riders
- Patients must pay part of this deductible themselves before insurance reimbursement begins
- Co-payment components remain, although typically capped
This means that even well-insured patients will experience having to pay a portion of their hospital bill out-of-pocket.
For major illnesses such as cancer, where treatment pathways can involve multiple admissions, scans, and therapies, the stage at which cancer is detected will significantly influence how much deductible and co-payment burden you may experience; which leads us to our next point about early detection.
New frontiers in early detection: The role of liquid biopsy
Traditional cancer screening targets specific organs, such as breast or colorectal screening. However, some cancers (especially the rare ones) lack effective screening tools.
However, emerging technologies such as liquid biopsy, which is a blood test that can detect tumour-derived DNA circulating in the bloodstream, aim to identify cancer signals across multiple organs earlier than conventional methods.
In Singapore, multi-cancer early detection tests developed by companies such as Lucence analyse genetic and epigenetic markers associated with cancer. If abnormal patterns are detected, the test can indicate the likely tissue of origin, guiding further evaluation.
While these multi-cancer early detection tests are not a replacement for established screening such as mammograms, pap smears, or colonoscopy, liquid biopsy may complement existing approaches and support earlier detection, particularly for cancers that typically present late.
Earlier detection means cancers may be found when:
- Tumours are smaller
- Disease is localised (has not spread)
- Treatment is simpler
- Cure rates are higher
- Costs are lower
Cancer screening options available in Singapore

Singapore’s national guidelines recommend age-appropriate screening for common cancers, including:
- Mammogram for breast cancer
- Colon screening for colorectal cancer
- Pap smear/HPV testing for cervical cancer
- Low-dose CT for selected lung cancer risk groups
Private hospitals and clinics in Singapore also provide comprehensive screening services, including:
- Radiology-based cancer screening
- Endoscopic screening
- Specialist risk assessment
- Genetic and advanced blood-based screening options
- Integrated diagnostic follow-up pathways
This integrated model allows patients with abnormal findings to transition quickly from screening to diagnosis and treatment which is a key factor in early-stage management.
What happens if a screening test detects cancer?
If a screening test, whether imaging, traditional tumour biopsy, or liquid biopsy, detects a possible cancer signal, the next step is diagnostic confirmation.
This may involve:
- Targeted imaging (CT, MRI, PET-CT)
- Specialist consultation
- Organ-specific tests
- Tissue biopsy
If cancer is confirmed, treatment planning begins. Depending on cancer type and stage, this may include surgery, radiotherapy, systemic therapy, or combined approaches.
While cancer screening itself does not treat the disease, it paves the way for early diagnosis and treatment, which in itself, is a step in the right direction for a good prognosis.
Will cancer screening and treatment in Singapore be covered by insurance?

If you have been diagnosed with cancer, the next obvious step is to wonder whether your cancer screening and subsequent care are claimable under insurance.
In Singapore, the distinction is important.
Screening tests
Most screening tests, including multi-cancer blood tests,
are considered preventive care and are typically not claimable under Integrated
Shield Plans.
However, certain nationally recommended cancer screening tests, such as mammograms, Pap smears/HPV tests, and colorectal screening, may be subsidised under government programmes (such as the Healthier SG programme) for eligible Singapore residents.
Diagnostic investigations after abnormal findings
Once a screening test
identifies a suspicious finding and a doctor orders diagnostic evaluation, imaging,
consultations, and biopsies are generally claimable under your Integrated
Shield Plan and MediShield Life,
subject to policy terms.
Cancer treatment
If cancer is diagnosed, treatment which includes
surgery, radiotherapy, chemotherapy, and approved cancer drugs, is typically covered under
Integrated
Shield Plans and riders, subject to deductible, co-payment, and drug coverage rules.
In Singapore, the ability to claim for cancer drug treatment is guided by the Ministry of Health’s Cancer Drug List (CDL), which specifies clinically proven and cost-effective cancer medications eligible for MediShield Life and Integrated Shield Plan claims. Coverage limits and claim amounts may vary depending on the specific drug and insurer.
Treatments or drugs outside the CDL may have reduced claims limit or require higher out-of-pocket payment, depending on your policy terms.
This means screening is usually self-funded (or subsidised under national programmes), but the downstream diagnostic and treatment pathway is largely insurable within policy and CDL frameworks.
In addition, patients with Critical Illness Insurance may receive a lump-sum payout upon cancer diagnosis, providing financial support beyond medical expenses.
What is the Cancer Drug List (CDL)?
The CDL is a national list of cancer
drugs approved for insurance claims under MediShield Life and Integrated Shield Plans. It
helps ensure patients have access to effective treatments while keeping premiums
sustainable.
Why early cancer detection lowers treatment costs
Cancer treatment intensity, and therefore cost, is strongly linked to stage at diagnosis.
Early-stage cancers often require:
- Limited surgery
- Shorter hospital stay
- Minimal systemic therapy
- Fewer scans
Late-stage cancers may require:
- Combination therapies
- Long-term drugs
- Repeated imaging
- Ongoing admissions
These differences translate into significant differences in cancer treatment costs.
Under the new rider structure, patients must meet part of their deductible before insurance coverage begins.
If cancer is detected early:
- Fewer treatments are required
- Total bill size is smaller
- Deductible burden is lower
Late-stage cancers often generate large bills quickly and repeatedly, increasing cumulative co-payments.
The earlier the cancer, the smaller the deductible journey.
Long-term cancer care: How long will insurance cover treatment?
Some cancers require prolonged or lifelong treatment, particularly metastatic or chronic cancers. And this is often a source of worry for cancer patients and their caregivers as they will worry about whether their insurance coverage has a time limit
In Singapore, Integrated Shield Plans generally cover medically necessary cancer treatment for as long as it remains clinically indicated, subject to policy terms.
However, several factors influence long-term coverage for cancer care:
- Policy remains in force
Premiums must continue to be paid and policy must not lapse. - Treatment is medically necessary
Therapy must be recommended by the treating specialist. - Drug coverage rules apply
Some cancer drugs are subject to Cancer Drug List (CDL) limits or claim caps. - Annual and lifetime limits
IP plans have annual claim limits (often $1–2 million) but no fixed time limit on duration of treatment.
This means that patients receiving ongoing chemotherapy, targeted therapy, or immunotherapy over years can generally continue to claim, provided treatment remains necessary and within policy coverage rules. Health insurance is designed to support both your acute and chronic cancer care.
Cancer-specific riders and additional protection in Singapore
Despite this reassurance that cancer treatment (though prolonged) can be covered by your standard health insurance, some people may still feel the need for additional support. Because cancer treatment is not always a one size fits all scenario, it is often very personalised. Therefore, some insurers in Singapore offer additional cancer riders or supplementary benefits designed specifically for cancer care.
These may vary by insurer and plan type but can include:
- Higher claim limits for cancer drug treatment
- Extended outpatient cancer therapy coverage
- Reduced co-payment for cancer treatment
- Lump-sum payouts upon cancer diagnosis
- Broader access to certain therapies
Such riders aim to reduce the financial impact of prolonged cancer treatment, especially if you require systemic therapy over months or years.
Critical Illness Insurance: Financial support beyond medical bills
In addition to the standard hospital insurance such as MediShield Life and Integrated Shield Plans, many Singapore residents also hold Critical Illness Insurance.
Unlike hospital plans that reimburse medical expenses, Critical Illness Insurance provides a lump-sum cash payout upon diagnosis of specified serious illnesses, including cancer (subject to policy definitions and stage criteria).
This payout can be used for anything, including:
- Income replacement during treatment
- Household expenses
- Supportive or non-claimable care
- Rehabilitation or recovery needs
- Out-of-pocket medical costs
Most new policies cover early-stage cancers, while others pay only for major or advanced cancer stages. Coverage scope and payout amounts vary across plans, so please remember to check with your agent or your policy contract.
Because cancer treatment may affect a your ability to work or generate income, Critical Illness Insurance helps soften the load by addressing the broader financial impact of illness beyond hospital bills alone.
So plans such as Critical Illness Insurance, Riders, and Cancer Riders complement rather than replace your standard Integrated Shield Plan.
Corporate health insurance: What it covers and what it may not
If you are a working adult in Singapore, you may also be covered under your Corporate Insurance. These plans may include hospitalisation and cancer treatment benefits, but coverage levels vary widely between employers.
Corporate Insurance may provide:
- Hospitalisation coverage during employment
- Specialist consultations and investigations
- Cancer treatment benefits within policy limits
- Access to private hospital panels
However, your corporate plan is tied to your employment. This means that your coverage will stop if you change jobs, retire, or leave the workforce, including during ongoing illness.
Additionally, the coverage limits are also typically lower than your personal Integrated Shield Plans, and long-term cancer therapy will most likely exceed annual corporate caps.
For this reason, personal health insurance remains essential you have a super comprehensive with corporate coverage.
Summary: Layered cancer coverage
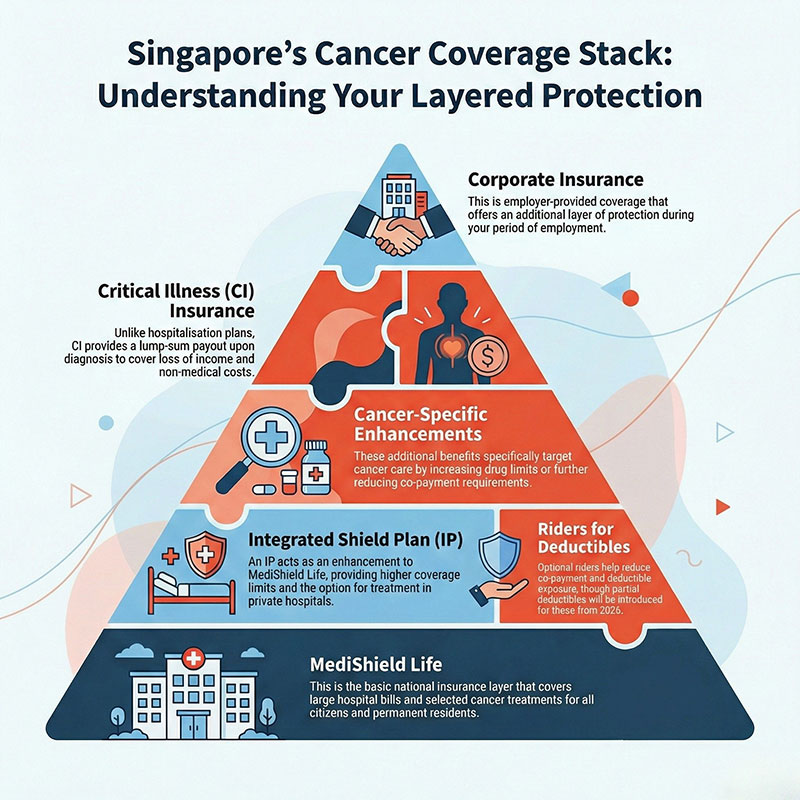
Understanding this coverage stack helps patients anticipate out-of-pocket exposure, especially for long-term cancer care.
Early detection saves lives and money
For decades, the message around cancer screening has been clear: early detection improves survival.
In 2026, another reality is emerging in Singapore’s healthcare landscape.
Early detection also reduces financial burden.
The earlier the cancer:
- The fewer treatments required
- The lower total cost
- The smaller deductible impact
- The shorter treatment journey
Cancer care will always involve uncertainty, but one factor consistently improves both outcomes and affordability: stage at diagnosis.
Early detection as financial protection in 2026
Although advanced screening tests may involve upfront personal cost, they function as financial risk reduction.
Detecting cancer earlier can:
- Reduce treatment complexity
- Shorten therapy duration
- Avoid prolonged systemic therapy
- Lower cumulative co-payments
- Limit deductible burden
Cancer care will always involve uncertainty, but one factor consistently improves both outcomes and affordability: stage at diagnosis.
Early detection saves lives and in 2026, it also saves money.
Know your coverage, before you need it
Not sure if your plan covers what matters most? Check how your current insurance stacks up using our Coverage Checker.





